This Simple Solution Could Sharply Lower COVID-19 Infections, Harvard Medical Doctor Says
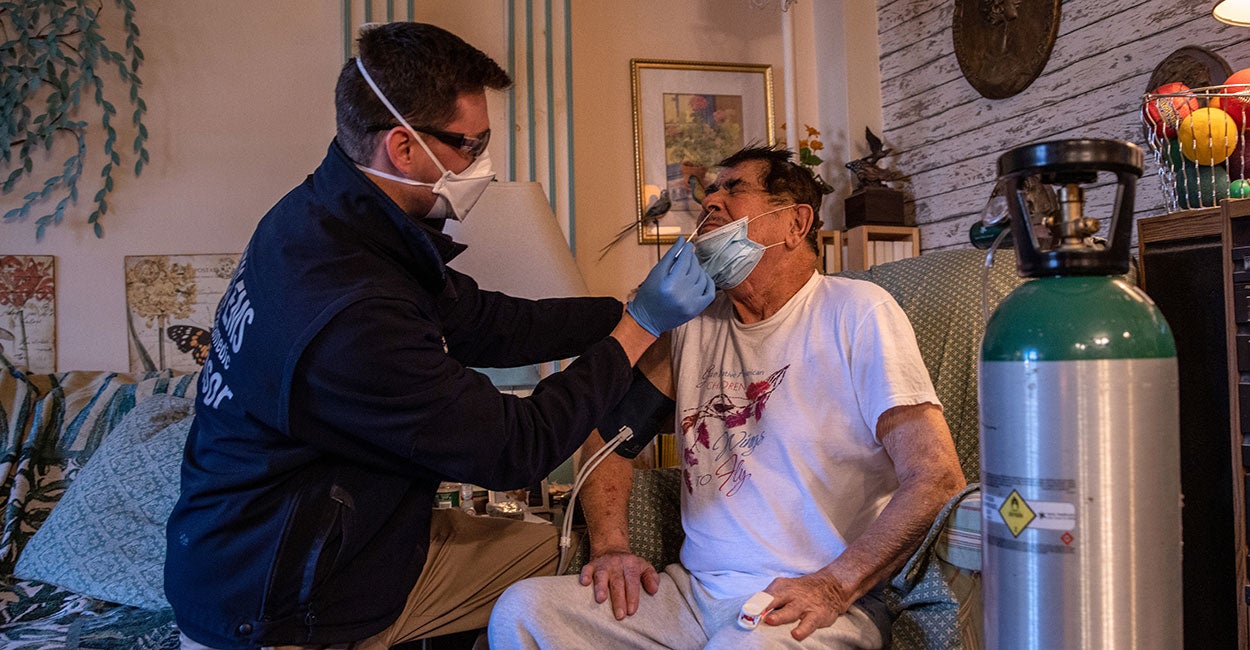
Dr. Michael Mina, assistant professor of epidemiology and immunology at the Harvard School of Public Health, joins “The Daily Signal Podcast” to discuss how rapid-result tests could dramatically decrease COVID-19 cases and allow much of the economy to reopen.
And Mina, who also is associate medical director of microbiology at Harvard Medical School, breaks down why these tests haven’t been made widely available, but should be now.
We also cover these stories:
- Lawyers for former President Donald Trump demand that his impeachment be dismissed, as the Senate impeachment trial is set to begin Tuesday.
- House impeachment managers release a fiery brief of their own, saying that “even after he incited insurrection, President Trump took numerous steps on January 6 that further incited the insurgents to escalate their violence and siege of the Capitol.”
- Rep. Ron Wright, R-Texas, just reelected to a second term, dies after contracting COVID-19. He also had battled lung cancer.
“The Daily Signal Podcast” is available on Ricochet, Apple Podcasts, Pippa, Google Play, and Stitcher. All of our podcasts can be found at DailySignal.com/podcasts. If you like what you hear, please leave a review. You also can write to us at [email protected].
Virginia Allen: I am joined by Dr. Michael Mina, an assistant professor of epidemiology and immunology at the Harvard School of Public Health and an associate medical director of microbiology at Harvard Medical School. Dr. Mina, thank you so much for being here.
Dr. Michael Mina: I’m very happy to be here.
TRENDING ARTICLES
Virginia Allen: You spoke at a Heritage Foundation event not long ago titled “Rapid COVID Tests: A Cure for Lockdowns, a Complement to Vaccines.”
The response to COVID-19, really across America, has so much so largely been to quarantine as much as possible, to wear a mask, social distance when you have to go out, and wait to be vaccinated. But, Dr. Mina, you propose that we actually have a much better and more effective solution that we really just haven’t taken advantage of. Could you explain what exactly that solution is?
Mina: Sure. Yes. The solution is, at its heart, effectively to empower people to know their own status. And by that I mean for people to understand, are they infectious right now? Do they have infectious virus in them that could be potentially harmful to others around them?
And the way that we could do this, the way that we could empower and inform people of whether or not they have infectious virus, is through the use of frequent rapid testing. Testing that people can perform at home, on their own terms, to know their status, to know, do they have the virus? Is it at a level, if so, that is infectious? And if so, to stay home that day, but do it on their own terms.
If they want to report, they could report voluntarily, but many people in this country don’t want to report their health status, and I think we have to respect that that is a position that many people hold and work with people, meet people where they’re at.
And allowing them to know if they are infected and if they are contagious with SARS-CoV-2, or the virus that causes COVID-19, is a tool that we could be using daily across the country right now, if we were to choose to act in that direction.
Allen: So explain just a little bit of the practicality of these tests. I mean, how complicated is it for someone to perform a test on themselves? How much would this cost? How would they be produced?
Mina: These tests are extremely simple. They are effectively like a pregnancy test. If you have two lines, you’re positive. If you’re one line, you’re negative.
The way that it works is you take a swab and you just swab the front of your nose. It’s not one of these really deep swabs that make you feel like you’re poking your brain. It’s just a shallow swab in the front of your nose.
You put that swab usually into a little tube of buffer or liquid, and then you put a couple of drops of that liquid onto a paper strip test, just like a pregnancy test.
So it’s extremely simple. Young children could do it. Adults could do it. Elderly people could do it.
The tests can be made in huge numbers. If we really try to build some of the most simple of these tests, we could be making tens of millions of these every day. We could have been doing this many months ago.
The technology is old. Like I said, it’s the same technology, just like a pregnancy test. It actually uses the same type of tools for it. The cost can be very low.
What I would personally like to see is the government make both purchases and essentially provide these to public health agencies, and the public health agencies provide them to people at home, through the mail, or however they get distributed. Maybe they’re distributed at your grocery store around the block.
But short of that, if we do land in an area where people ultimately have to pay for them, they can be $4 or $5 a piece. I think at scale, they can come down even further. Two dollars a piece per test is not an unreasonable amount to consider that we could get to with scale.
Allen: During the Heritage Foundation event a few weeks ago discussing these tests, you said that, really, ideally, we would see Americans maybe taking a test about twice a week.
So if all Americans were taking an at-home COVID test twice every week, and then were choosing to stay home if that test came back positive, how quickly would we actually, in theory, begin to see a dramatic decline in positive cases?
Mina: If we actually had most Americans using a test like this twice a week, we would see a decline overall in this country by 50% or 60% in a couple of weeks—by more than that in a month, and by two months into such a rigorous testing program, the outbreaks would go away.
This is something that I call public health testing. It’s not medical testing. It’s not diagnostic testing. The goal of public health testing or public health screening is to essentially stop outbreaks from spreading. The way that this works is an outbreak will only spread if you infect more people than who are currently infected.
So if you have 100 people infected today and those 100 people go on and infect 130 people, then the outbreak escalates exponentially. And after four weeks in that scenario, you’d have 500 new infections, four weeks later.
On the other hand, if you can just get 100 people to infect 90 people, and you do that for a few weeks in a row, then all of a sudden, instead of 100 people getting infected each day, you have 30 people getting infected each day.
So the relative gain, it’s a 90% reduction against what we have now. And that’s just if 100 people infect 90. With this type of testing, we could absolutely get to 100 people infecting 40 new people. …
Even if half of the population chooses not to participate or just chooses to throw their results away and say, “I don’t care. I’m still going to work,” or, “I’m still going to church,” it would still be enough to actually get that R-value, get 100 people to infect fewer than 100 people.
We don’t have a long way to go to get there, and these tests would make all the difference between exponential increases in cases versus exponential decay of outbreaks.
Allen: You’re really on the front lines of researching this virus, of researching solutions. At what point in your research did the lightbulb kind of go off of, “This is the answer”? And then why does it seem like the rest of the medical community, the [Centers for Disease Control and Prevention] is not really getting behind this?
Mina: This became pretty readily apparent back in April for me, and I started publishing on it back then. And I also started publishing back then on the PCR test and why the PCR test was kind of being misunderstood.
The problem, and the reason I bring PCR up, is we have this incessant sort of continued and persistent infatuation with the PCR test.
The PCR test has to be done in a laboratory. It takes days to get results back. It takes [an] amazing amount of manpower and expertise to run these labs. We’re never going to scale up in the way that we actually need to tackle an outbreak.
The PCR test is a medical test. It’s designed to diagnose people so that when I put on my physician hat and a patient comes to me and says, “Dr. Mina, I haven’t been feeling well for two weeks,” I want to be able to use a test that I can tell my patient, “It looks like you have had COVID recently, or maybe have it today.”
But for public health, that’s not the right test for public health. We need a test that is fast, that can be used frequent enough to actually catch people when they’re transmitting, and that is accessible. And we don’t want a test that stays positive for weeks after somebody is infectious.
The PCR test, unfortunately, stays positive for weeks after people are infectious, and the [Food and Drug Administration], as well as, unfortunately, our CDC and others, continue to require that all of these rapid paper strip tests, which are also called rapid antigen tests, the requirement is that they get compared to a PCR test out in the world in order to be authorized.
And what that means is that if I have already recovered from COVID, my PCR test today might stay positive. But if I use one of these rapid antigen paper strip tests, it should be negative, but the FDA would look at that result and say, “Aha, the paper strip test failed. We’re not going to authorize that.”
But from my personal perspective, I would say, “No, it’s succeeded. I have already gotten over my infection. I don’t want a test that tells me that I need to continue isolating. I want a test the tells me if I need to isolate today, not if I needed to isolate two weeks ago.” So there is a disconnect.
The science is so clear. We know PCR stays positive for so long, but the FDA to this day requires that every test be compared against the PCR.
I’ll give a very quick example of how ridiculous this is.
If I am an X-ray machine company and I’m going to the FDA, and I say, “FDA, I want to create this new X-ray machine and put it into hospitals. It’s good for tracking people with pneumonia, or whatever the reason, or broken bones.”
… The equivalent situation is the FDA would say, “That’s not good enough, because we just saw how good an MRI machine does, and your X-ray is not good enough.”
They’re different purposes. The speed and the accessibility are wholly different, and, unfortunately, the FDA has not been able to understand this.
Allen: Well, it just seems so illogical. I’m feeling frustrated just hearing you explain the fact that this is such an obvious solution, and yet no action has been taken on it.
So what does need to be done, whether maybe, I don’t know if it’s members of Congress or individuals in the medical community, to really put pressure on the Food and Drug Administration, on the Centers for Disease Control and Prevention, and say, “Hey, this actually is a legitimate solution and we need to move forward on it”?
I mean, is there anything that at this point can really get this train moving in the right direction?
Mina: Now, I have published on this in the top journals in the world. Scientists know about this. Physicians generally have heard about it. But there’s so much confusion because most people don’t really understand the science of testing, even though all you really have to know is what I just explained to you, which is, it’s really a pretty simple concept at heart.
To be honest, I’m not quite sure what the best avenue is. Is it to continue having scientists kind of try to rally around us? I don’t think that’s going to work. I think what really needs to happen now is we need Congress, we need Senators, we need governors. We need the president’s administration. As high as it needs to go.
We need people to recognize that the science exists, recognize that there is a void, a misinformation, and a misalignment of priorities at the FDA at the moment, where the FDA is prioritizing medical diagnostic tests that I would want if I’m a hospital director, and they are not able to see their way to a test that is designed specifically to stop transmission at the community level, and to open up schools and businesses.
So I think what we need is some pressure being applied to say to the FDA, “Look, you’re doing a wonderful job evaluating medical diagnostic tests, but now it’s time to create a new pathway at the FDA that also is able to evaluate tests in the context of public health.”
We have not seen that yet, but what we do know is that at least at this moment in time, the president has stated that he wants a rapid test to be a large part of a program forward.
So now we really need to see the action toward that, and part of that action is ensuring that the test we have today, that can be used in the tens of millions today on American soil, are actually getting evaluated and put out as fast as possible.
Allen: Dr. Mina, practically speaking, what is the cost of actually getting these tests mass produced and then into the homes of Americans all over the country?
Mina: If the government were going to actually pay for all of this, it would cost about $20 billion—$20 billion would get us to a point where every American could have these tests on a routine basis in a sufficient quantity, say twice per week, and where we could actually stop the spread of this virus.
But in my opinion, $20 billion is not a lot of money here. It’s a drop in the bucket compared to the $16 trillion price tag that this virus has. It’s 0.1%, essentially, of the price tag of this virus, and it would get us to a place where we could potentially, actually, completely control the epidemic and the outbreaks on our soil.
It is not only, however, left to the government to make all the purchases. There are major multinational and international companies that are absolutely willing to pay for these tests to keep their offices open, to keep their employees employed. I’m actually already working with some to do clinical trials since they’re not FDA-approved yet.
So I think that we would see a combination of the government stepping in to pay for some of it, and we would also see massive investments from companies that they recognize that it’s absolutely worth their while to keep their employees safe, to make their environments as safe as possible.
Allen: Are you optimistic that we’ll be able to actually see some action and movement forward on this, and that this might still be something that can take place where we are able to mass produce these tests and distribute them?
Mina: I do think so. I certainly hope so. I think we are starting to see now increased movement to really get them starting to be built.
Unfortunately, the government is currently still blocking the biggest companies that are able to really make these tests in the highest scale. They are investing in certain tests that aren’t public health tests, that just aren’t going to scale, like the Ellume test that came out.
It’s a great test, but it’s the kind of test that should live in a pediatrician’s office. It will not be used frequently. It’s too expensive. … It’s got circuit boards and batteries in every single one, and they all get thrown away. But we just invested a lot of money into that.
Ultimately, for enough tests, that will be, essentially, a drop in the bucket for our needs.
So I think that priorities haven’t been fully aligned and really planned out, but I do believe we’re starting to see an increased understanding that rapid tests are crucial.
The faster you get results, the faster you can stop spread, and I hope that we continue to see some movement, but I really do believe we need Congress to be up in arms about this. This is a tool that could keep everyone’s constituents safe, within weeks.
Allen: It’s definitely, obviously, impossible to know what could have been, but if we went back to March or April, right at the kind of the onset of the spread of COVID-19, and right away these tests were produced, were distributed to Americans, even people all over the world, at this point, where do you think we would be in the fight against the virus, if we had done this, had these rapid response tests available to individuals from the onset?
Mina: You know, we would have had an extremely different fall. I believe very firmly that our fall, which has been, I think, by all accounts, absolutely horrendous, I don’t think anyone can argue with that. We have seen hundreds of thousands dead as a result of this, and lives destroyed, businesses destroyed.
Had we started using these tests back in April or May, even June or July or August, when cases were pretty low in much of the country or just starting to pick up again, we would have not seen those outbreaks pick up.
And that’s the whole idea of keeping that R-value below one. Keeping for every 100 people who are infected, have them infect fewer than 90. You can still have 90 new infections occur, but as long as that’s lower than the number of people who are infected in the last generation, the outbreak will not happen.
So we wouldn’t have seen these rises in cases. We wouldn’t have seen us hit 300,000, 400,000 new cases per day. It could have been 20,000 new cases per day through the whole fall with minimal mortality. We would have seen a very, very different picture had we started this at the beginning of last summer.
We did an economic evaluation of this with Harvard economists and, ultimately, we found that with an investment of between $20, at that point, we were being conservative, so we actually said $50 billion, but I hold that we do not need $50 billion to do this, … the return on investment, we would have saved at least half a trillion dollars in that had we done that, and probably more. We were being very conservative with it all.
So lives would have been saved. We would not have seen the massive destruction we’ve seen. We could have potentially seen an environment where stores remained open through the holidays and cases would have been overall low enough that people are just going about their day.
Twice a week, they spend 30 seconds and run their COVID test after they brush their teeth, and that is enough to stop this outbreak from continuing to persist.
Allen: Before we let you go, I do want to ask for your thoughts on the vaccine. The vaccine has begun to be distributed, but we are hearing a lot of mixed things, a lot of different opinions on it, and I know many Americans are hesitant to take it. What are your thoughts on the vaccine?
Mina: Well, I want to be very clear for anyone who’s hesitant, the vaccine is very safe. We have seen huge numbers of vaccines be given out. Millions, and millions, and millions. It is an extremely safe vaccine.
Unfortunately, the extremely rare events that occur make headlines. But if we put it in the context of car accidents, and we put a car accident on every headline, every time one happens, we would think that driving is extremely unsafe when it is extremely safe.
So I want to be very clear that I would personally, and I have, I recommend to my family to get them. I’ve looked at the safety profiles of them.
I believe that the vaccine is not going to be the end-all, be-all of this pandemic. My grave concern is that we will see vaccine immunological escape, meaning the virus learns to mutate in such a way that the vaccine really loses some of its effectiveness.
And if we see that, we could find ourselves in a very difficult position where we are trying to then decide, “How do we vaccinate people with new versions of the vaccine? Do we give the new versions to people who have already been vaccinated or to people who have not yet received even one vaccine?” It will create a lot of problems if we have to go in that direction.
Allen: Certainly. Well, we so appreciate your time. We appreciate you being on the front lines and all of the research that you’re doing. How can our listeners follow your work and stay informed of that research that you’re doing?
Mina: Well, I’m very active on Twitter. My Twitter handle is @MichaelMina_Lab. And I’m often writing op-eds or quoted in the national media, but really, I would say, don’t follow me.
I mean, you can definitely follow me on Twitter if you want, but what I would really like is for people to write to their congresspeople, people to write to their senators, phone your governor, whatever it takes, and demand that you understand the reality of paper strip testing and rapid testing at home, and that you want that type of test, if you do, that is.
That this is a tool that is meant to empower you. This is a tool that is meant to give you information, to let you know if you are a danger when you go to your parents’ house for dinner.
We have to stop this rote idea of just, “Nobody can do anything social for the next year or two.” It is destructive to our society. That’s a major component of public health, is still psychological health, and we have to find other avenues to keep people safe while we continue with society, how we know it.
And I think that these tests can make everyone safer to go to work, to go to school, to go to church, to go shopping. They will improve the safety, and they will reduce the burden of this virus on society.
I hope that people let their representatives and elected officials know that that is what they’re asking for.
Allen: Dr. Mina, thank you so much for your time today. We truly appreciate it.
Mina: Absolutely. I’m very happy to have joined you.

Read the first chapter of The Woketopus right now for FREE
Today, even with President Trump’s victory, leftist elites have their tentacles in every aspect of our government.
The Daily Signal’s own Tyler O’Neil exposes this leftist cabal in his new book, The Woketopus: The Dark Money Cabal Manipulating the Federal Government.
In this book, O’Neil reveals how the Left’s NGO apparatus pursues its woke agenda, maneuvering like an octopus by circumventing Congress and entrenching its interests in the federal government.
You can read the first chapter of this new book for FREE in this eBook, The Woketopus: Chapter One using the secure link below.
TRENDING ARTICLES

The Daily Signal depends on the support of readers like you.